The Transfer of Health Information to the Provider and the Transfer of Health Information to the Resident at Discharge are MDS, process-based measures. The Transfer of Health Information measures look at the transfers of a resident’s reconciled medication list to the subsequent provider and/or to the resident. These measures impact the SNF QRP and Care Compare.
These quality measures look at SNF Medicare Part A stays ending in a discharge to another setting. The stay is defined as the time from resident admission or re-entry to the facility as identified by a 5-day PPS Assessment to Part A PPS Discharge.
The numerator for both quality measures is the number of stays for which at the time of discharge, the facility provided a current reconciled medication list to the subsequent provider and/or to the resident, family and/or caregiver, respectively.
The completeness of the reconciled medication list is left to the providers and resident who are coordinating care. There is guidance available on what to include in the Reform of Requirements for Long-Term Care facilities at Federal Register: Federal Register :: Medicare and Medicaid Programs; Reform of Requirements for Long-Term Care Facilities. Documentation sources for the reconciled medication list can be electronic and/or on paper and may include such items as discharge summary records, Medication Administration Records, home medication lists, and physician orders.
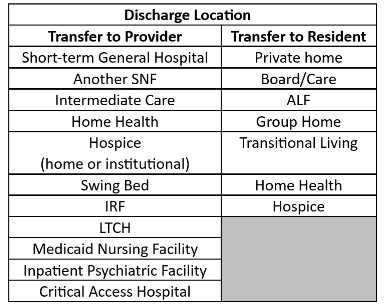
The denominator for the measures is the total number of SNF Medicare Part A covered resident stays ending in discharge to another setting. The variation in the denominators for these 2 measures is based on the discharge setting. Transfer of Health Information to the Provider is assessed for both institutional and home settings, while Transfer of Health Information for the Resident is assessed for those going to a home typesetting.
This measure is calculated quarterly and includes all SNF stays during the quarter eligible for inclusion in the numerator. Each stay for a resident with multiple stays is counted. Also, neither of these measures are risk-adjusted or stratified.
The calculation for this measure is as follows:
- Determine the denominator count (MDS item A2105: number of resident stays based on discharge location; as noted above the responses counted will vary depending on which measure is being calculated – to subsequent provider or resident).
- Calculate the numerator count (MDS item A2121 = 1 and/or A2123 = 1: Total number of stay where a reconciled medication list was transferred).
- Calculate the facility observed score (divide the numerator count by the denominator count and multiply by 100).
For this measure it is critical we are coding discharge location (A2105), whether the facility provided a reconciled medication list to the subsequent provider and/or the resident, family, and/or caregiver (A2121/A2123), and route of transmission (A2122/A2124).
In comparison to other measures, these are relatively straightforward quality measures which can have a big impact for the resident with a smooth transition to subsequent care and a hopefully successful discharge to home.
To learn more go to IMPACT Act of 2014 Data Standardization & Cross Setting Measures | CMS