The short-stay quality measure related to Outpatient Emergency Department Visits is a Claims and MDS Based Measure impacting Care Compare and Five Star. The measure is titled the Percentage of Short-Stay Residents Who Have had an Outpatient Emergency Department Visit.
The numerator for this measure is the number of stays where a resident had 1 or more outpatient claims for an Emergency Department (ED) visit, regardless of diagnosis, within 30 days of an entry or reentry. This would include visits occurring after discharge from the nursing home if within the 30-day time frame. Visits are not counted if the thru date on the ED claim is equal to the from date on an observation stay claim or an inpatient unplanned hospitalization claim.
The denominator for this measure includes beneficiaries enrolled in both Part A and B Medicare who entered or reentered the nursing home from a hospital and who were not enrolled in hospice during their facility stay or identified as comatose, as per the MDS admission assessment.
The denominator is the number of eligible nursing home stays meeting the following criteria:
- Stays preceded by an inpatient hospitalization, within one day of the stay start date, as identified by the Medicare Part A claims stay dates
- Beneficiaries are identified using the CMS Enrollment Database. Those enrolled in a Medicare Advantage plan for any part of their stay or who were not enrolled in both Medicare Parts A and B for any part of the stay are excluded.
- Stay is excluded if the ‘from’ and ‘thru’ dates overlap with a hospice claim.
- Stay is excluded if the resident is noted to be comatose on the MDS (B0100 = 01) or if the information in B0100 is missing from the MDS.
- Stay is excluded if it cannot be linked to an MDS assessment within 14 days of the start of the stay, or if data is missing from the MDS related to the numerator, the denominator or risk-adjustment.
The exclusions are indicated in the criteria above.
The risk-adjusters for this measure include both claims-based and MDS-based covariates. The following are the claim-based covariates:
- Age
- Sex
- Length of stay during the hospitalization before stay
- Time spent in Intensive Care
- Medicare enrollment for disability
- End-Stage Renal Disease (ESRD)
- Number of acute care hospitalizations in the 365 days prior to the stay
- Principal diagnosis
- Outcome-Specific Comorbidity Index
The MDS-based covariates include the following:


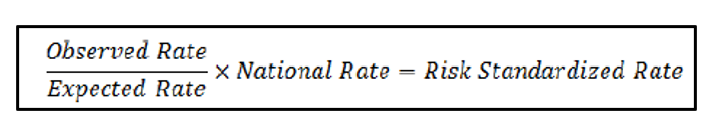
For this measure, a National Rate, an Observed Rate, and an Expected Rate are determined to arrive at a Risk Standardization Rate.
Teamwork among the Interdisciplinary Team is critical to limiting emergency room visits. A proactive approach through continual monitoring, screening, assessment, and communication regarding a resident’s condition can limit outpatient emergency room visits.
To learn more about this Quality Measure and more, go to Quality Measures | CMS.