The Quality Measure for Number of Hospitalizations per 1,000 Long-Stay Resident Days reviews unplanned hospitalizations of long-term residents to ensure nursing homes are evaluating and caring for residents who are admitted to the nursing home from the hospital. This Claims Based Measure impacts Nursing Home Care Compare and Five Star.
This measure examines the number of unplanned inpatient admissions or outpatient observation stays for long-stay residents of a nursing home during a 1-year period.
The numerator includes the number of long-stay residents with an admission to an acute care (ACH) or critical access (CAH) hospital for an inpatient or outpatient observation stay. This does not include planned inpatient admissions. Planned discharges are identified using the principal discharge diagnosis category and the procedure codes from the inpatient claim. If a resident is enrolled in hospice, unplanned inpatient admissions and observation stays are excluded, and not counted.
The numerator for this measure is calculated using the same algorithm as CMS’ Planned Readmissions for the Short-Stay hospital readmissions measure. As stated above, the algorithm uses principal discharge diagnosis category and procedure codes listed on inpatient claims as coded by the AHRQCCS software. Regardless of diagnosis, observation stays are included in the measure.
Exclusions include:
- Between admission and discharge or end of the target period, whichever comes first: Resident was not a Medicare beneficiary and/or Resident was enrolled in Medicare managed care during any portion of the stay
- Resident enrolled in hospice care
- Resident not in the nursing home for any reason during the episode, including days admitted to an inpatient facility or other institution, or days temporarily residing in community


This measure is risk-adjusted. The covariates for risk-adjustment are as follows:
- Age, sex, and race/ethnicity categories
- Number of ACH stays in prior 365 days before the day the resident became a long-stay resident
- Outcome specific comorbidity index with diagnoses pulled from inpatient claims 365 days before the day the resident became a long-term resident
There are covariates based on responses on the MDS as well.
Functional Status
- Rarely/never makes self-understood by others (B0700)
- Cognitive status moderately impaired, severely impaired, assessed by staff, or not assessed (C0100 – C1000)
- Rejected care for past four to seven days (E0800)
- Wandering once or more in the past week (E0900)
- Walks in room independently or with supervision or limited assistance (G0110C1)
Clinical Conditions
- Shortness of breath with exertion (J1100A)
- Shortness of breath when lying flat (J1100C)
- End-stage prognosis (J1400)
- Internal bleeding (J1550D)
Clinical treatments
- Anticoagulant received (N0400E)
- Antibiotic received (N0400F)
- Diuretic received (N0400G)
- Chemotherapy for cancer (O0100A2)
- Radiation for cancer (O0100B2)
- Oxygen therapy (O0100C2)
- IV medications (O0100H2)
- Transfusions(O0100I2)
- Hospice care (O0100K2)
- Isolation/quarantine for active infectious disease (O0100M2)
- Speech therapy (O0400A4)
- Respiratory therapy (O0400D2)
Clinical diagnoses
- Gastroesophageal reflux disease or ulcer (I1200)
- Ulcerative colitis, Chron’s disease, or Inflammatory bowel disease (I1300)
- Neurogenic bladder (I1550)
- Multidrug-resistant organism (MDRO) (I1700)
- Septicemia (I2100)
- CVA, TIA, or stroke (I4500)
- Quadriplegia (I5100)
- Multiple Sclerosis (I5200)
- Parkinson’s disease (I5300)
- Anxiety Disorder (I5700)
- Respiratory failure (I6300)
Other
- Entered facility from a psychiatric hospital (A1800)
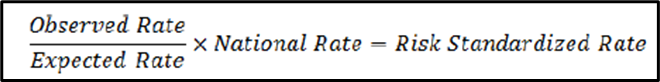
For this measure, a National Rate, an Observed Rate, and an Expected Rate are determined to arrive at a Risk Standardized Rate.
Teamwork among the Interdisciplinary Team is critical to limiting hospitalizations. A proactive approach through continual monitoring, screening, assessment, and communication regarding a resident’s condition can limit unplanned hospitalizations.
To learn more about this Quality Measure and more, go to Skilled Nursing Facility (SNF) Quality Reporting Program (QRP) | CMS.